Wednesday, January 18, 2006
Anesthesia Blood Loss
-
Printer Friendly|#| Trackback
Anesthesia-related blood loss almost never exceeds surgical blood loss...but it can. I recently had a case where the IV tubing became disconnected from the IV hub during a case. The blood pressure cuff was on the same arm, and the intermittent tourniquet effect of the cuff cycling served to increase venous pressure sufficiently to cause blood to flow backward and out the now disconnected IV.
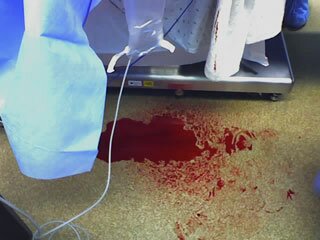
But wait, there's more. The patient was receiving the medication that kept her asleep through her IV and the disconnect put her at very real risk of waking up or having awareness in the middle of her surgery. This apparently did not happen in this case based on my interview of the patient in the recovery room, but it surely could have.
This misadventure would have been entirely avoided by the use of IV tubing with a locking hub (often called a Leur-Lock connector) connecting the IV tubing to the IV hub. In our case, someone decided the locking connectors were not worth the extra cost and our connections were just slip fit (no lock). How many times should this happen before the equipment is changed?
This has happened many times to my colleagues and I (though usually not with such blood loss), each time we complained, were told it was being looked in to, but kept getting the same connectors. I took the above rather striking photograph to some clinical managers, who agreed we needed to change, and said that they had already ordered the new tubing. Until it arrives, I'm starting IV's myself so that I can use locking connectors.
Thursday, December 22, 2005
Misconceptions about why anesthesia is safer
-
Printer Friendly|#| Trackback
Walter Olson has taught me much about the legal system as it pertains to medicine via the PointOfLaw forum. I have to take exception with a post made today however. In pointing to an article that considers whether the lessons of patient safety in anesthesiology are generalizable to other fields of medicine, he writes:
"Incidentally, because anesthesiologists are now more vigilant than ever not to court an overdose risk by giving patients any more than the minimum they need, there is apparently a rising incidence of the phenomenon of "anesthesia awareness", in which underdosed patients are actually aware of the surgery in progress and perhaps end up undergoing psychological trauma as a result. So what happens next? You guessed it."
Overdose risk is not and was never a cause of patient morbidity and mortality in my field. Second, it is not at all clear whether the 'rising incidence of the phenomenon of anesthesia awareness' is anything but a) better reporting (i.e. you don't find what you don't look for) b) realization among patients that there's something else they can sue for or c) an effort by one medical device company which makes depth of anesthesia monitors to panic hospitals and anesthesia groups into buying their product (a product which, by the way, has not been shown to decrease the incidence of awareness).
The specialty is actively engaged in evaluating this 'problem' with the same approach it has used to improve patient safety in other areas such as airway management and positioning injuries.
Thursday, December 1, 2005
How do you mark a surgical site?
-
Printer Friendly|#| Trackback
The American Academy of Orthopaedic Surgeons has a policy on marking surgical sites titled Guidelines for Implementation of the Universal Protocol for the Prevention of Wrong Site, Wrong Procedure and Wrong Person Surgery. It's worth reviewing and comparing to your institutions policy. For example:
- Make the mark at or near the incision site. Do NOT mark any non-operative site(s) unless necessary for some other aspect of care.
- The mark should be unambiguous (e.g., use initials or "YES" or a line representing the proposed incision; consider that "X" may be ambiguous).
- The person performing the procedure should do the site marking.
There's much more to the guideline, but your current policies are most likely to be at variance with the above three points. One of the surgery centers I work at, for instance, marks the surgical site with an 'X'. I've explained to them that 'X' is ambiguous (does X mark the spot, or does X mark 'not this one'?) and even explained the details of a malpractice case in which marking with an X came into play. Another hospital was in the habit of marking both sides ('L' and 'R'). Also confusing. Finally, several centers have the nurse preparing the patient for surgery to mark the site. Also not a good idea.
Saturday, March 12, 2005
Obstetrical deaths in the UK--Anesthesia component
-
Printer Friendly|#| Trackback
Why Mothers Die 2000-2002 - Report on confidential enquiries into maternal deaths in the United Kingdom
Chapter 9--Anaesthesia
The anesthesia chapter concludes:
"The management of haemorrhage is a shared responsibility of midwifery, obstetric, anaesthetic and blood transfusion personnel. Anaesthetists should be ready to suggest that the obstetrician summons help in the face of major haemorrhage regardless of the obstetrician’s grade or experience. Good communication is vital and regular practice of emergency drills is crucial, particularly in units with a high turnover of staff."
I would like to think that many of the problems pointed out in this report would not happen in the United States, but that would be intellectually dishonest. If you provide anesthesia for obstetrical patients as I do, it's worth reading over this report for the lessons that are applicable in the US.
Senate Committee Approves Bill To Establish Medical Error Reporting Database
-
Printer Friendly|#| Trackback
Kaisernetwork.org--Capitol Hill Watch | Senate Committee Approves Bill To Establish Medical Error Reporting Database - :
" The Senate Health, Education, Labor and Pension Committee on Wednesday approved by voice vote a bill (S 544) that would create a database to allow care providers to report medical errors, CQ Today reports. The database would be used to track medical errors, examine trends and prevent reoccurring mistakes, CQ Today reports. Information included in the database would not be used in medical malpractice lawsuits, according to CQ Today. Before the full Senate considers the measure, committee Chair Michael Enzi (R-Wyo.) and Sen. Edward Kennedy (D-Mass.) are expected to insert language to clarify that the bill would not affect information already available to attorneys for use in malpractice suits. The committee last year approved similar legislation, which was unanimously approved by the Senate. The House approved a separate version of the legislation, but the issue died after conference committee members were not appointed. The new bill is expected to pass the Senate. The House Energy and Commerce Committee has not yet scheduled a review of the bill (Schuler, CQ Today, 3/9). "
Friday, January 21, 2005
'X' Marks the Spot. Or Does It?
-
Printer Friendly|#| Trackback
Newsday.com has details of a recently announced jury verdict in a case of wrong side surgery:
" "A Manhattan hospital and the chief doctor for the New York Rangers hockey team were ordered Thursday to pay a dance director and choreographer a total of $450,000 because the physician operated on the man's wrong knee.
The jury awarded the money to Douglas Hall, 43, who entered St. Vincent's Hospital on Nov. 30, 2001, for arthroscopic surgery on his right knee. Despite marking that knee with an 'X,' Dr. Andrew Feldman operated on the left knee. " "
Does an 'X' mean 'operate on this one' or does it mean 'do not operate on this one--operate on the other one'? I've seen a few patients write 'No!' on the non-operative side. We all got a chuckle out of it, but it worked! Rather than an 'X', the mark should be placed on and refer to the correct side--either 'R' or 'L'.
The rest of the article points out that the OR was also set up for the wrong side. Just another example of multiple failures being needed for a medical misadventure to occur. I'm sure there was no end of the 'blame game' going on for this one.
Tuesday, November 9, 2004
Anatomy of a Near Miss
-
Printer Friendly|#| Trackback
Medical errors are insidious. Many, many errors occur that do not lead to a bad outcome, but they are errors nonetheless. Given a different patient or set of circumstances, those same errors could result in injury, death, or at the very least less than optimal care. The following example serves to reinforce this point.
A thin, elderly woman is admitted the morning of her planned multi-level spinal laminectomy, instrumentation, and fusion. She is healthy, active, and appears younger than her stated age. She meets her anesthesiologist for the first time twenty minutes before the case. Upon review of her records, she appears to be free of cardia or pulmonary disease, but he notes laboratory results on the chart which indicate a macrocytic anemia (blood count of 30--normal is greater than 35 or so). The patient does not recall being told this before. No mention is made of this finding in the surgeon's history and physical examination, or elsewhere in the chart. Someone did think to do serum B12 and folate levels, both of which were found to be normal but no note is present to indicate the differential or planned workup. The finding is discussed with the surgeon and the case proceeds.
Error number one: the abnormal laboratory value should have triggered further evaluation. Some evaluation was attempted, but there was nothing in the chart to indicate by whome, or what their conclusion was. Significant blood loss is likely in this case. Starting with a lower hematocrit means less blood can be lost before a transfusion becomes necessary.
Error number two: the anesthesiologist should have cancelled this case due to a new anemia of unknown etiology. The severity of the anemia is such that a blood transfusion will almost certainly be needed. If time had been taken to evaluate and treat the anemia, the blood count may have risen sufficiently to reduce the likelihood of needing a transfusion. Even if the blood count could not be improved, directed donation or intraopoerative blood salvage techniques could have been used. Why didn't the anesthesiologist cancel the case? No good reasons, just all the usual ones. He was afraid the surgeon would be angry. He kne w the patient had been dealing with severe pain and was holding out just for this surgery.
Intra-operative blood loss was approximately 700 cc. Euvolemia was maintained with Hespan and lactated Ringer's solution. The patient was warm, urine output was good, and both blood pressure and heart rate were stable. Her hemoglobin near the end of the case was now 7, and a unit of blood was ordered from the blood bank. When no blood arrived within 30 minutes, the blood bank was called to inquire if there was a problem. No blood sample from the patient was available in the blood bank to cross-match bank blood against. A sample was immediately drawn into a red-top vial and sent. The case ends, patient is extubated successfully, and transported to the recovery room where her vital signs remain stable and urine output good. The anesthesiologist continues with other scheduled cases after giving report and asking the recovery room nurse to administer one unit of blood when it become available.
After another thirty minutes pass, the blood bank calls the recovery room to inform them that the sample was received in the wrong vial. The blood bank used to require a red-topped vial, but now want a lavender-topped vile (the former contains no anticoagulant, the later does). A phlebotomist is called to draw the new sample and the patient received a blood transfusion fully two hours after the anesthesiologist made the decision to administer blood.
Error numbers three through ten: 'what we have here is a failure to communicate.' There was a failure to communicate:
- that blood had not been drawn pre-operatively as ordered (even though the pre-op checklist indicated it had)
As an interesting aside, this was the first morning the nurses in the pre-op area were asked to use a computerized nursing record rather than their preferred paper method of charting.
- that the blood bank had no specimen to crossmatch blood against after receiving a call for blood.
- that a change had been made in what kind of specimen was needed for crossmatch.
- you can fill in the remainder.
The only reason this patient did not suffer harm from this incident is that she was physiologically very healthy. Imagine a patient with stable but significant coronary disease. That patient would not have tolerated a hemoglobin of seven so well. Imagine a more significant blood loss. It's better to be lucky than good. It's even better to be both.
This example demonstrates what is so often true of medical misadventures: it is a series of events
in combination which conspire against the practitioner and the patient to cause harm.
My response to this event is to draft a 'Go/No-Go' list. My personal decisions on whether to do a case is heavily influenced by what I know the surgeon reaction will be. I'm not saying that's the right reaction, mind you. It's just my reaction (in wanting to please people as I do). A Go/No-Go list is similar to what NASA uses to decide whether or not to launch a space craft. If any item is 'No-Go' the launch is scrubbed. On my anesthesia Go/No-Go list, if I discover an item in a patient chart that's on my list, launch is scrubbed and the case is rescheduled. New, unexplained anemia is certainly on that list, especially in light of a surgery likely to result in significant blood loss. I need to spend some serious time adding to this list. I'll post it as a work in progress.
| 1 |
2 |
3 |
4 |
5 |
6 |
7 |
| 8 |
9 |
10 |
11 |
12 |
13 |
14 |
| 15 |
16 |
17 |
18 |
19 |
20 |
21
|
| 22 |
23 |
24 |
25 |
26 |
27 |
28 |
| 29 |
30 |
31 |
|
|
Dec Feb
|
